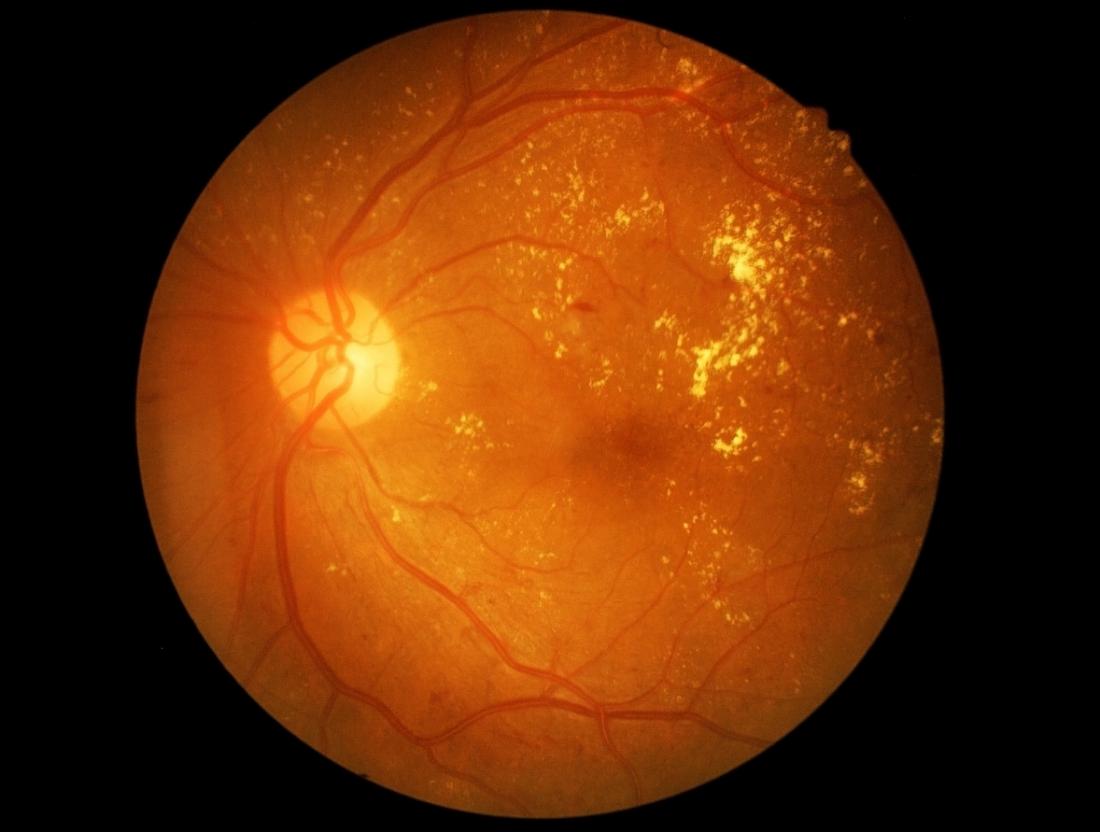
A healthy retina is necessary for good vision. For diabetic retinopathy patient, at first they may notice no changes to the vision. But over time, diabetic retinopathy can get worse and cause vision loss. It usually affects both eyes.
Specifically, diabetic retinopathy is a microangiopathy (microvascular disease) primarily affecting pre-cappilary arterioles, capillaries and post capillaries venules, although larger vessels may also be involved (the high blood sugar levels damage the capillaries, or tiny blood vessels, that supply blood to the retina). It will also exhibit both features of microvascular occlusion as well as leakage.
Usually, the symptoms found in diabetes retinopathy are asymptomatic in the early stages, nor pain, blurred vision may occur when the macula swells from leaking fluid and vision is blocked if new blood vessels grow on the surface of the retina and bleed into the eye. Generally, diabetic retinopathy can be classified into:

SYMPTOMS OF DIABETIC RETINOPATHY
Typical symptoms of retinopathy include:
- Sudden changes in vision
- Blurred vision
- Pain in the eye
- Seeing spots
- Loss of vision
- Double vision
- Floaters in your vision
- Night visision loss
Complications of retinopathy in later stages can include blindness or retinal detachment.
(Seeing spots)

Generally, treatment for diabetic retinopathy (DR) depends on type, severity and previous treatments of DR. Treatments are most effective when DR is detected early, so it’s important for diabetics to have routine eye exams.
As a conclusion, regular or routine eye check up by licensed optometrist will help to detect diabetic retinopathy at its earliest stage and subsequently helps to prevent further damage to the eye’s retina.